Dementia is a neurodegenerative disease that represents more than just memory loss because it generates a decline in the person, undermines his or her independence, and negatively affects his or her health and quality of life.
The management of incontinence in an elderly person with dementia is very complicated and can be highly emotionally delicate. Caregivers often feel overwhelmed by the constant work of care and support, especially if they are caring for their own family member, and over time find themselves facing destabilization in their personal lives. In many cases, they wonder whether it is worth continuing in this way or it would make more sense to get help and entrust their loved one to a nursing home.
The goal of this article is to help the caregiver have a more peaceful life and to help the caregiver cope better with daily life through small steps.Two simple things you can do to improve your loved one’s lifestyle and routine are to encourage proper nutrition and to tie physiological needs to moments of daily routine. Also, to increase the personal safety of the caregiver, it is important to make the bathroom clearly visible and accessible. It is important to take care of skin care on a regular basis using specific and quality products. From a psychological point of view, empathic and communicative care is equally important, making one’s loved one feel understood and understood.In the next paragraphs we go into much more detail through 7 useful tips on how to put these arrangements into practice.
Table of Contents:
- Living with dementia is a challenge
- What causes urinary incontinence in people with dementia?
- At what stage of dementia does incontinence occur?
- 7 tips for caregivers
- Get help

Image 1: Caregiver caring for an elderly person.
Living with dementia is a challenge
Dementia afflicts more than 1 million elderly people in Italy and leads to loss of cognitive and motor skills. An estimated 3 million people are directly or indirectly involved in the care of their loved ones. We are talking about thousands of families who suffer physically and psychologically on a daily basis.
In fact, dementia not only has implications in the life of the elderly person, but it also causes suffering, frustration and distress in family members. Caring for one’s parent, seeing his or her mental and physical state constantly worsening is not an easy process to deal with. Often one does not feel up to the task and all this leads in many cases to high levels of stress or worse to severe depression.
What causes urinary incontinence in people with dementia?
One of the most common problems with advancing age is incontinence, in fact after age 60 between 15% and 35% of the elderly in Italy begin to suffer from it. These rates rise significantly in the elderly with dementia, up to 60-70% of cases. Several studies also show us that a high percentage of these, about 75/80%, are RSA residents therefore many more than those domiciled at home.
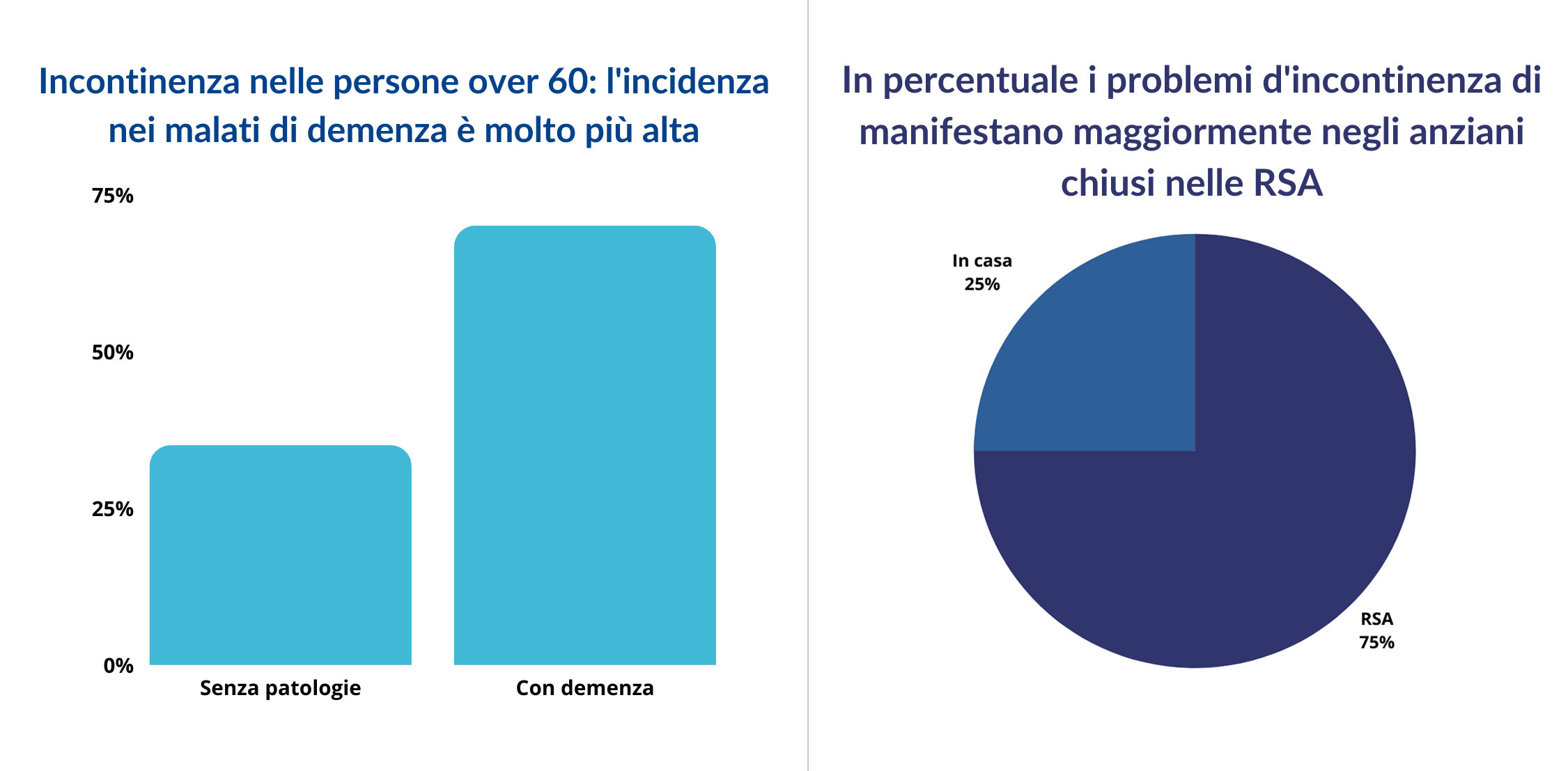
Chart 1: Among people over sixty, incontinence mainly occurs in the elderly with dementia
In people with advanced dementia , incontinence is due to a mix of factors, both physical and mental. Bowel and bladder control is often lost due to the inability to react quickly to stimuli or to remember where the bathroom is. In severe cases, the physical and mental perception of urgency to urinate or bowel movements vanishes.
In general, the reasons that cause incontinence in people with dementia are:
- Physical limitations in reaching the bathroom on time
- The loss of mobility
- The feeling of confusion that leads to not recognizing the bathroom or not remembering how to reach it
- Communication difficulties with the caregiver
At what stage of dementia does incontinence occur?
Generally, the first cases of incontinence begin to occur in the intermediate stages of the disease, mainly due to mental blackouts.
It is at this stage that the elderly person begins to have the first instances of disorientation, confusion, times when one may forget where the bathroom is located, to not remember well how to use the proper accessories or even urinate and defecate in places that are not the right ones.
These can be compounded by physical issues, such as difficulty in undressing, undoing buttons, or a general disregard for one’s personal hygiene.
In the more advanced stage of the disease, on the other hand, the elderly person incurs much more frequent and prolonged episodes of disorientation in which he or she is not aware of his or her surroundings, does not recognize signals given by his or her body such as urgency in having to do his or her needs, and develops severe difficulties in communicating this need.
At this time the person loses perception of the problem and becomes totally dependent on someone, a caregiver who will have to take care of him or her continuously.
7 Tips for caregivers
Incontinence is recognized by caregivers as the biggest problem in managing an elderly person with dementia.
It is good, at the onset of symptoms, to seek medical attention to see if there are physical issues behind these difficulties, otherwise it can be very helpful to follow these 7 tips that can significantly improve the lives of both of you.
1: Make the bathroom easily recognizable, accessible and usable
It sounds trivial, but the elderly with dementia especially in the later stage have difficulty reaching the bathroom due to a physical impossibility or they may not remember where it is located, even in their own home.
These are ten tips that can be critically important for the elderly person’s safety:
- Make the bathroom visible by always leaving the door open
- Attach photos on the door and use strong colors so that it stands out from the surrounding walls
- Create a comfortable and fragrant indoor environment that entices the person to stay there for as long as necessary
- Make sure the door is easily opened
- Rearrange spaces so that the bathroom is as close as possible to the resident’s bed.
- Always leave a light on at night
- Install support handles, perhaps colorful, that the elderly person can hold onto to prevent falls
- Remove all obstacles both external and internal, such as plants, trash cans, and items that might be mistaken for a toilet
- For men, it can be especially helpful to fix the toilet at the right height and color the water inside to create contrast and make it easier to distinguish
- Hide or disguise the bidet to prevent it from being confused with the toilet.
2: Ensure the hygiene and cleanliness of the caregiver and the place where he or she lives
The skin of the elderly is very fragile, and incontinence can weaken it even more, becoming a cause of skin irritation and injury.
This happens because of prolonged contact of urine and/or feces with your loved one’s skin. Fragile skin, having a poor physiological protective barrier, is more prone to the onset of injury. Injuries are easily penetrated by bacteria that can cause irritation or infection.
It is therefore essential to properly wash the elderly person, check that his or her skin is perfectly dry and that he or she always has clean clothing to wear
Many experts recommend using no-rinse products because they allow the elderly person to wash without continually using water that could damage the skin.
For cleaning, it is preferable to use soft disposable cloths which provide better hygiene than classic sponges and, due to their high absorbency and durability, ensure dry and lint-free skin.
Another important aspect is to try to have the caregiver live in an environment that is safe, pleasant and clean. To do this, it is important to clean and ventilate rooms regularly, eliminating possible sources of odors.
Cleaning of clothing, bedding, as well as chair covers and mattresses is essential. For everyday items that cannot be washed consistently and conveniently (chairs, sofa, mattress…), it is recommended to use covers made of special waterproof and breathable materials.

Image 2: Caregiver caring for an elderly person.
3: Use the most appropriate products for the elderly person
Using the right products represents a key element that can help as much decrease the possible occurrence of incontinence-related skin problems, ensure greater cleanliness and safety and, of course, facilitate the work of the caregiver. It is very important:
- Choose clothing that is easy to remove and clean.
For example, you could have people use pants with elastic bands instead of zippers, which are considerably easier to undo. Pants with button closures, complicated zippers, and narrow openings should be avoided. Elderly people may have physical difficulties in removing clothes, which may cause them to be slower to reach the bathroom. Of course, for the caregiver this also results in huge savings in terms of time and also physical.
Often elderly people with dementia tend to want to remove clothes or diapers, even at inappropriate times. So it would be appropriate in these cases to use clothes that cannot be removed without help, perhaps with a back zipper.
- Have the caregiver wear diapers.
Even in the absence of actual incontinence (urinary and/or fecal), it is recommended to use absorbent pants, which prove essential when difficulty in reaching the bathroom arises. There are various types, very comfortable to wear both disposable and washable and reusable.
Pants or diapers should be changed as soon as one notices that they are soiled,, generally every three hours to avoid prolonged contact with liquids and bacteria, except at night where it can be kept longer so as not to interrupt sleep.
Proper fastening of these restraining devices is also essential. This is because in case of too loose fastening there is the risk of embarrassing leakage or that the elderly person can easily remove it while in the opposite case it could cause redness and abrasions on the skin of the caregiver.
- Use skin care products daily.
Leaks due to incontinence can cause skin irritation in the long run, and in severe cases, injury. It is therefore good to create a daily routine, using a variety of products that can make it easier for the caregiver to have healthier and more moisturized skin. These products should be used after each evacuation or urination thoroughly.
Fundamental is the choice of these products (creams, cleansers and shampoos) and the methodology of use and application, which must be done with gentle movements. Also very important is the drying phase, which must be thorough and performed by patting the skin, without rubbing. The barrier creams are very useful for protecting the skin from prolonged contact with moisture and irritants.
4: Encourage proper nutrition and hydration
Having proper nutrition is a vitally important factor that avoids unpleasant repercussions in the already complicated management of incontinence. There is a whole range of beverages and foods that an elderly or incontinent person should not consume because they lead to an increase in the frequency of the need to go to the bathroom by increasing the occasions of discomfort.
Very important is to ensure proper hydration, making sure that the caregiver takes in the correct amount of fluids.
While recommending a consultation with one’s General Practitioner, a generalized indication might be this:
| Foods to avoid | Recommended Foods |
| Coffee | Fish with omega 3 (cod, salome, swordfish) |
| Tea | Whole foods (bread, pasta, rice, oats, barley) |
| Chocolate | Yogurt and fermented milk |
| Carbonated beverages | Fruits in season (apples, bananas, grapes, persimmons, strawberries) |
| Spicy foods | Green leafy vegetables (broccoli, turnips, lettuce, spinach, asparagus) |
| Dried fruits | Legumes (chickpeas, beans, fava beans, quinoa, etc.) |
| Alcohol | Soy |
| Some acidic foods (lemons, limes, oranges, grapefruit) | Water (1.5/2 liters per day) |
| Tomato products | Cheese (to flavor dishes without using spices) |
| Sugar, honey and sweeteners in general | Vegetables (cucumbers, peppers, carrots, pumpkin) |
Table: list of foods that can help or harm people with incontinence
Obviously not everyone reacts in the same way to the administration of these foods, so if they are part of the elderly person’s diet, it is important to try to reduce them individually, trying to assess what the body’s response to that change is on a case-by-case basis.
5: Try to establish periodic urination
Trying to create a routine can be a great help because it allows the body to get used to certain rhythms.
In general you should try to encourage bathroom use as soon as they wake up, after meals and before bedtime. When they are still fairly independent, you can ask them to go to the bathroom every two hours or so, figuring out what is the perfect timing for their body.
In the more advanced stages of the disease, the caregiver is unable to manage his or her impulses on a regular basis. At this stage, lack of communication could be an obstacle, so common nonverbal forms must be found that can indicate the need for bathroom use.
When the elderly person loses the communicative and physical ability to provide for his or her own needs The caregiver should then be responsible for accompanying the elderly person to the bathroom every few hours, usually two, and always try to do so at the same times.
We imagine this can be quite complicated so it is essential to ask for help from professionals or other family members who can help.
6: Detailed care of pelvic emptying.
The caregiver should be skillful, as mentioned earlier, in trying to establish a good routine. However, he or she should also help the caregiver to carry out the practice of urination and evacuation properly and then monitor it in terms of both quantity and quality. There are several aspects that the caregiver should monitor.
- The caregiver must sit correctly on the toilet. This is an essential aspect because it ensures that there is proper emptying of the bladder and rectal ampulla.
- The caregiver should not push in an attempt to stimulate or speed up urination or evacuation.
A good caregiver must therefore be able to succeed in establishing a routine in urination and evacuations, monitoring that these are carried out in the correct way and creating a kind of planned emptying. If this is done in the right way, the results can be great for both the caregiver and the elderly person, resulting in fewer accidents and less stress and fatigue for the caregiver.
7: Be empathetic, understanding and communicative
The last piece of advice is not related to physical issues, rather it focuses on the importance of emotional support to the elderly person.
The person with dementia needs to be reassured and comforted; it is important for the caregiver to try to give serenity to the caregiver, show approval for what he or she is doing, and especially not make the caregiver feel guilty when incontinence episodes occur. It may seem that the caregiver does not realize or feel emotions, but in many cases they feel humiliated by what is happening.
One should not regard this topic as taboo, rather one should talk about it and always have a positive and understanding attitude toward the caregiver.
It is necessary to realize that not everyone reacts in the same way to these inconveniences. Some may get nervous and be grumpy, while others may recognize the problem as part of their illness. Therefore, it is important to genuinely approach the situation and be respectful, talk calmly about the topic and avoid coming across as rude and nervous.
Choose empathy instead of pity, trying to understand their feelings and thoughts and instilling positivity. This can definitely help you in the long run.
They often feel awkward, try to encourage communication, and if they are reluctant you start the conversation clearly and make it clear that you are fully aware of their problems and needs. Stay positive and patient even when an incident occurs.
Get help
Managing an elderly person with dementia also causes great distress, especially in the case of caring for a loved one, perhaps a parent. Seeing him or her in that condition can be lacerating and frustrating. All these elements can impact so much on the caregiver’s life, cause stress and in many cases even depression.
However, one must understand that it is not a problem to take a break and not be there every day. There is nothing wrong with asking other family members or more experienced people for help. On the contrary, it is absolutely necessary to take time off, perhaps vacation time to regenerate yourself as much mentally as physically so that you will be more efficient when you return to care for the person with dementia.
