There are many factors that can cause irritation and damage to the peristomal skin.
The worst thing is that many ostomates often tend to think that skin changes cannot be cured, but this is not the case.
If you happen to struggle with redness and irritation around the stoma, then you are reading the right article!
In this article you will find a comprehensive guide that will help you easily recognize and treat any peristomal complications; in addition, you will find pictures of the most common cases of peristomal skin irritation and also tips on how to prevent and manage these problems.
If you are curious about almost are the most common skin changes that occur around the stoma, we give a brief explanation below:
Table of Contents:
- What is peristomal skin irritation: how to detect and manage it
- 1. Irritant dermatitis caused by chronic leaks.
- 2. Excessive bleeding
- 3. Seborrheic dermatitis
- 4. Pressure ulcer
- 5. Folliculitis
- 6. Hypertrophy/Hyperplasia – Papillary alterations.
- 7. Candidiasis
- 8. Peristomal hernia
- 9. Allergic dermatitis with skin redness
- 10. Redness due to aggressive removal of the collection system (mechanical injury)
- Peristomal skin color changes: what does it mean?
- 9 tips to prevent damage to peristomal skin
- Frequently asked questions
The most common signs of irritated peristomal skin or infected ostomy may be itching, dryness, or color changes. The most common infections and irritations, on the other hand, are irritative or allergic dermatitis and fungal infections, such as candida.

*This survey was conducted in May 2021 and was answered by 38 people of different nationalities. The survey was posted in the following ostomy-specific Facebook group:
What is peristomal skin irritation: how to detect and manage it
The skin around the stoma should look similar to the skin on the rest of the body, and the stoma should have a pink color, similar to the inside of the cheeks. Therefore, if you notice a change in color, or if you experience pain or itching, it is very likely that your peristomal skin is irritated or damaged.
Read on to find out what the 10 most common peristomal complications are.
Remember: to prevent any kind of irritation, it is essential to employ and master a good hygiene routine. To achieve this goal, we have prepared a step-by-step guide to help you better manage the care of your peristomal skin and achieve healthy skin and ostomy.
Read on to find out what the 10 most common peristomal complications are.
1. Irritant dermatitis caused by chronic leaks.
Irritant dermatitis is considered one of the most common peristomal skin complications and tends to develop due to constant leakage under the plaque. The effluents (which are highly irritating) come into contact with the stoma causing various skin problems.
If you want to learn more about leakage, we provide all the information about it at this article.
Irritant dermatitis usually occurs when:
- The cut-out hole of the adhesive plate is too large compared with the stoma
- plaque is not properly applied to the peristomal skin
- ostomy bag leaks
Signs and symptoms:
- At an early stage, the peristomal skin will appear inflamed: skin redness/eruption, swelling, pain, itching.
- In a secondary stage, if the leaks continue to occur for a long period, blisters may appear and could lead to loss of skin in the affected area (ulceration). The longer the contact with the effluent, the worse the damage to the peristomal skin will be.
Management:
- Treatment should begin by identifying the reasons behind the leakage.
- Check periodically whether the garment adheres properly to the skin
- A garment that does not adhere well and causes leakage should be changed immediately to protect the peristomal skin and prevent further damage.
- Clean the skin with warm water and a cleanser with a self-balancing pH. We recommend using the cleanser Bioderm Stoma Plus, as it was developed exclusively for ostomy hygiene and helps take care of sensitive and irritated skin.
- To absorb moisture from the injured peristomal skin, you can use ostomy powder. In addition, you can also use a moldable ring, which will provide a good adhesive surface on which to place your garment.
Recent studies show that the use of self-balancing pH soap restores the optimal pH of damaged skin and, together with the isodermic cream, provides rapid improvement, within 3-6 days after the first application.
In fact, a daily moisturization of the skin with this dermoactive cream has been shown to protect and heal sensitive scalps from irritation.
2. Excessive bleeding
The stoma has many blood vessels at the top, which can bleed easily while changing the pouch and cleaning the surrounding skin.
If the stoma starts bleeding, first try to determine where the bleeding is coming from and the severity of it.
- If it is minor bleeding from the edges of the stoma, you can solve the problem by gently dabbing the ostomy with a soft, clean, dry cloth. We recommend using Bioderm Superabsorbent Wipes.
- In case the bleeding persists for several minutes or worsens, seek immediate medical attention.
- If the excessive bleeding comes from within the stoma, then:
- could indicate intestinal bleeding. This could be due to portal hypertension, liver disease, some medications (such as anticoagulants), and some blood diseases that prevent blood clotting.
Therefore, it is important to seek immediate help from your referring physician.
- at times, you might notice the contents of your sac a reddish color and automatically you might think of internal bleeding however, if you have recently ingested foods such as sugar beets or a red Gatorade, then don’t worry, it will almost certainly be a false alarm.
3. Seborrheic dermatitis

Seborrheic dermatitis is a common skin disease that not only affects various sites on the body (such as scalp, behind the ears, nose, chest, armpits, and navel), but also affects the skin around the stoma.
Signs and symptoms:
They appear as reddish spots on fair skin and light-colored spots on darker skin, with itchy, scaly scale formation.
Management:
- You can use an antifungal medication (spray or powder). Also, you can use a spray with hydrocortisone for topical use.
Be sure to let these products dry thoroughly before applying your new ostomy garment.
- You can also use this treatment to manage other parts of the body affected by seborrheic dermatitis.
4. Pressure ulcer

Excessive pressure on the peristomal skin could cause this type of skin problem. Many ostomates have contracted this type of ulceration after prolonged use of convex plaques.
Signs and symptoms
Early symptoms of a pressure ulcer often include mild discomfort or pain with redness around the peristomal skin. So if you should notice any discomfort when applying your ostomy garment, remove it and in about two minutes the problem should go away.
Often when these discomforts occur, skin changes such as pressure ulcers may occur if a quick solution is not used.
Management:
- If you use an ostomy belt, it is possible to solve this problem by loosening the pressure of the belt or even removing it completely to prevent further peristomal skin changes.
- Pressure ulcers often occur due to the use of an inappropriate ostomy garment. Therefore, try using a different collection system. (Consult with your referring physician or stomatherapist, especially if you are using an ostomy device with a convex plate, to see which collection device might be best for you.)
- To treat a peristomal skin ulceration, consider using hydrocolloid dressings.
5. Folliculitis
Folliculitis consists of inflammation of the hair follicles below the adhesive plaque.
This problem is much more common among males because they have more abdominal hair.
The main causes are:
- excessive sweating
- very high outdoor temperatures
- skin trauma due to actions such as shaving with a disposable razor blade or frequent removal of ostomy garment (which tends to cause tear folliculitis).
Signs and symptoms:
The most common symptoms of folliculitis are papules (small red bumps) or pustules (like small pimples) that cause skin redness and mild pain.
Management:
- Folliculitis can be managed with the use of the cleanser Bioderm Stoma Plus. Carefully wash and dry the peristomal skin, then apply a small amount of antibacterial powder before donning the new ostomy collection system.
- In addition, we recommend that you use an electric razor, following the direction of hair growth. Alternatively, use scissors with a rounded tip. After shaving, wash the peristomal skin thoroughly with a self-balancing pH cleanser and rinse with plenty of water.
- Avoid shaving with a razor or depilatory creams; these methods could cause micro-lesions and skin infections.
- However, if you decide to use either of these two ill-advised methods, consider using an ostomy powder or a moisturizing cream with a self-balancing pH, free of mineral oils, to revitalize the skin after shaving.
6. Hypertrophy/Hyperplasia – Papillary alterations.

Generally, this change appears around the stoma and is the consequence of prolonged irritation of the peristomal skin caused by frequent leakage below the plaque.
Signs and symptoms:
Hypertrophy, or papillary hyperplasia, consists of the appearance of tissue that appears “warty” (wart-like papules and nodules) or irregular around the stoma, with white, gray, or reddish-brown discoloration. In addition, it may bleed if you touch it.
Management:
It is important to use a collection system that fits your ostomy well. Therefore, be sure to measure it often.
- Use barrier rings to create a homogenous surface around the stoma.
- If you have a urostomy, maintain a urine pH of 6.0. You can do this by taking in more fluids and increasing urine acidity (drinking blueberry juice or taking vitamin C).
- Apply vinegar poultices (½ vinegar, ½ water) for about 10 to 15 minutes to the affected area, each time the pouch is changed, then pat the area dry before applying the new pouch.
These vinegar poultices are not dangerous to your health and have powerful antimicrobial capabilities. - Your referring physician may decide to cauterize your skin alteration with silver nitrate.
7. Candidiasis

Candidiasis tends to develop below the adhesive barrier because it is a very moist area.
It is usually caused by:
- leakage below the plate
- excessive sweating of the skin
- The administration of systemic broad-spectrum antibiotics
- skin hygiene with an antibacterial cleanser, which could damage the skin and create a perfect environment for fungal microbes to develop.
Signs and symptoms:
Candida appears as erythema with many scattered papules or pustules, and there is often an intense itching and burning sensation on the peristomal skin.
Management:
- Wash the peristomal skin with a little water and dry it well.
- Use an antifungal medication and make sure the skin has absorbed it completely before applying your collection system.
- If you cannot find an antifungal spray, buy the powder version (remember to wipe off excess, however, before applying your bag).
Do not use antifungal creams or ointments, as they may interfere with the adhesive power of your collection garment.
8. Peristomal hernia
A peristomal hernia occurs when, for various reasons, heavy pressure is applied from within the abdomen (such as in the case of a chronic cough, lifting too heavy loads, or fluid retention).
Signs, symptoms and management
Peristomal hernia appears as a protuberance or bulge around the stoma.
Take a look at your ostomy and check the following:
- If your ostomy is pink to red in color and is still functioning, then it is not an emergency and you can reduce it in the following ways:
- Apply gentle pressure or wear an ostomy support belt.
- If you are using a two-piece system, try one-piece system to get a clearer view of your hernia.
- If you are used to irrigating your ostomy, you should consider discontinuing this procedure, to encourage natural evacuation.
- If your stoma is bluish in color and you experience frequent severe abdominal pain, nausea and/or vomiting, and constipation, then you should seek medical attention immediately because these are clear signs of an emergency.
9. Allergic dermatitis with skin redness

Allergic dermatitis consists of a skin reaction to chemical allergens in the collection system you use. Normally, the materials from which ostomy garments are made are well tolerated by your skin. However, the allergy could be caused by the adhesive substance. Another possibility, is that the allergy is triggered by cosmetic products such as deodorant, fragrances, or skin cleansers that are not ostomy-specific.
Signs and symptoms:
The peristomal skin will appear reddish and you may experience severe itching, pain, and develop blisters and ulceration.
Allergic dermatitis is often easy to spot because it takes on the same size and shape as the adhesive plaque.
Management:
- You can manage allergic dermatitis with a topical hydrocortisone spray. Make sure the product is well absorbed into the skin before you apply your medical device.
10. Redness due to aggressive removal of the collection system (mechanical injury).

Mechanical injuries occur when:
- You remove the ostomy garment without paying much attention, causing skin injury.
- You change the collection system too frequently.
- Excessive rubbing is exerted during peristomal skin cleansing.
Signs and symptoms:
The affected area will appear red and be painful, with possible ulceration.
Management:
- You can treat this redness by using an ostomy powder. Once applied blow off the excess and let it dry before placing the new collection system.
Peristomal skin color changes: what does it mean?
Pink peristomal skin
The skin around your stoma should look similar to the rest of the skin on your abdomen. You may notice it a little reddened right after removing the adhesive plaque, but the color of your skin will most likely resume its normal color after a few minutes.
Red peristomal skin
Reddened peristomal skin may indicate possible irritation. In this case, it is important to identify and manage the problem before the situation worsens.
Bluish or purplish peristomal skin
If the skin around the stoma is bluish or purplish, it could indicate the presence of peristomal varices. This means that there has been dilatation of the veins around the stoma.
Very dark peristomal skin (dark red to black)
When the stoma appears very dark in color, it could be ischemia or necrosis of the ostomy (insufficient arterial blood supply to the ostomy site, causing death of the stomatal tissue).
Contact your referring physician immediately if you notice your peristomal skin is very dark in color.
9 tips to prevent damage to peristomal skin
It is essential to pay special attention to the following points, because these preventive measures are essential to care for the peristomal skin and avoid any possible complications:
- Replace your collection system regularly and check for leaks.
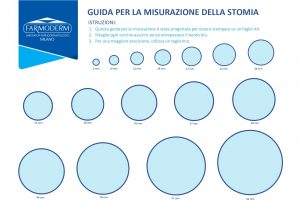
- Measure your ostomy periodically: as your stoma shrinks in size during the first few weeks after surgery, you should measure your ostomy frequently to adjust the size of the plaque opening with each pouch change. This will allow you to fit the ostomy correctly and avoid skin complications, such as irritation from leaks.
Download one of two guides to facilitate measurement:
Guide for measuring circular stoma
Guide for measuring the stoma ovale
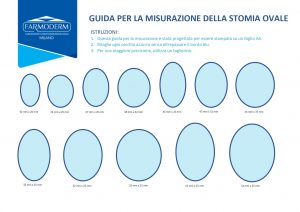
- Consider the use of adhesive removal products: if you find plaque removal difficult, there are many products that facilitate this procedure and, at the same time, will help you avoid injury to the peristomal skin.
- Use a cleanser and cream with a self-balancing pH and rinse thoroughly. Avoid using oily and alcohol-based products, as well as deodorants, perfumes or any product that might cause irritation. We recommend using. Bioderm stoma Plus e Bioderm dermocrema as both products are designed exclusively for the care of the ostomy and surrounding skin. With their unique self-balancing pH value formulas, they help prevent and treat any skin irritation without hindering the adhesive properties of plaque.
- Consider changing the type of plaque you use to another product if you notice you are allergic to it. Also, try testing the ostomy adhesive product on other parts of the body when you first use it (epicutaneous test).
- Dry the peristomal skin gently and slowly to ensure that no residue is left behind and that the skin is not irritated. It is essential to dry well to achieve good adhesion of the adhesive plaque and to prevent fungal infections (candidiasis). We recommend using Bioderm Superabsorbent Wipes. These wipes are extremely soft, durable and absorbent, making them ideal for all dermatological treatments with liquids, creams, oils or foams and the gentle cleansing of fragile or irritated skin.
- Dry the collection system thoroughly after showering, swimming or any exposure to water.
- Regularly check the color of your ostomy , which should be between pink and red. It should be very similar in color to the inside walls of your cheeks.
- Remove peristomal hairs periodically with an electric razor in the direction of hair growth.
Final considerations
We hope this information will help you manage and care for your ostomy.
Proper treatment will enable you to achieve, in a short period, positive results that will facilitate your daily life.
Frequently asked questions
Still can’t find the answer to your question? We have collected the most frequently asked questions related to peristomal skin irritation.
What is the best way to prevent itching around the stoma, peristomal erythema, and leakage from under the plaque?
Choosing the right collection system can help prevent itching around the stoma and leakage (you can try using a convex plaque). Also, correctly cut out the hole for your adhesive plaque, this way you can avoid many complications.
Why does my ostomy burn?
If your stoma or surrounding skin is burning, it could be a symptom of irritation or infection. Often, irritation of the peristomal skin is due to frequent contact between effluent and the ostomy; in other cases, this burning is due to allergic reactions to one of the components of the pouch.
What is a partial-thickness wound?
A partial-thickness wound occurs when there is a loss of the upper layers of the skin (epidermis, dermis, or both). It will look like an abrasion, blister or superficial ulcer. It happens when the skin comes into contact with irritants such as effluents or cleansers that are not ostomy-specific.