Is your ostomy very swollen and does it tend to protrude more than usual? Most likely you are very frightened, however don’t worry, an ostomy prolapse is not dangerous to your health.
Often, with the right care, a prolapse can be managed without the need for surgery.
It is important for you to know that in addition to corrective actions, there are also preventive actions you can practice, to avoid the risk of prolapse.
Here is how to manage a stomal prolapse: To treat a prolapse, try the following: lie down for 20 minutes, apply light pressure to the end of the stoma, use a cold pack to apply to the ostomy bag, for 20 minutes. If your stoma is still prolapsed, contact the hospital for targeted prolapse management .In addition to explaining what a prolapsed stoma is, we will tell you what the symptoms and causes are. In addition, we will explain prevention techniques to significantly reduce the risk of a prolapsed stoma.
Table of Contents:
- Definition: what is an ostomy prolapse?
- Symptoms: what does an ostomy prolapse look like?
- Causes: what causes prolapse of an ostomy?
- Risk: How high is the risk of developing a prolapse?
- Treatment: how do I grest a prolapsed ostomy?
- Medical management: when should I contact a doctor?
- Prevention: how can I prevent ostomy prolapse?
- Living with a prolapse: what should I do?
What is an ostomy prolapse?
An ostomy prolapse occurs when the intestine protrudes from the stoma opening more than expected, abnormally. This stoma protrusion can range in length from 2-3 cm to more than 10 cm.
What does an ostomy prolapse look like?
The symptoms of a prolapsed stoma are varied and diverse, and may appear singly or simultaneously, these are:
- swollen stoma
- telescopic protrusion
- stoma protrudes more than usual
- Stoma color changes: purple, dark red or light pink
- the stoma feels very cold to the touch
The appearance of a prolapsed stoma can change depending on position; for example, it may protrude when you are standing or sitting, but return to normal when you lie down.
What causes an ostomy prolapse?
An ostomy can prolapse for a variety of reasons; the most common are:
- L‘flu or other illness causes the patient to sneeze or cough a lot; this increases abdominal pressure and can push the intestines out of the stoma.
- The patient does very strenuous abdominal exercises or lifts too heavy weights. This increases pressure around the peristomal area, which can cause bowel protrusion.
- Pregnancy. A growing fetus will push other internal organs and increase the risk of a prolapsed stoma.
- The patient develops a tumor in the abdominal region.; as in pregnancy, a large enough tumor in the abdomen can push the internal organs, thus pushing the intestines out of the stoma.
- The muscles abdominal muscles of the patient are underdeveloped, as in infants; in infants or people whose abdominal muscles are underdeveloped, the abdominal wall may not be able to hold the bowel in place, and this can cause stomal prolapse.
- Obesity; excessive weight gain can increase abdominal pressure and cause telescopic protrusion of the stoma.
- The opening created during surgery for the stoma is excessively large.
How high is the risk of developing a prolapse?
Stoma prolapse represents one of the most common late complications, occurring in 1-16% of ostomized patients. The risk of prolapse differs among different types of ostomies and the age of patients.
Between 1998 and 2000, a U.S. study (with 204 participants who had an ileostomy or colostomy).
In this study, the risk of developing a prolapsed stoma was found to be 22 percent for adults and 38 percent for children.
In addition, it has been found that the risk is higher for people who have or have had a loop colostomy or ileostomy.
We conducted a similar survey where we asked people with an ostomy, “Have you ever had an ostomy prolapse? If yes, please indicate your type of ostomy,” and the results that emerged confirmed the above:
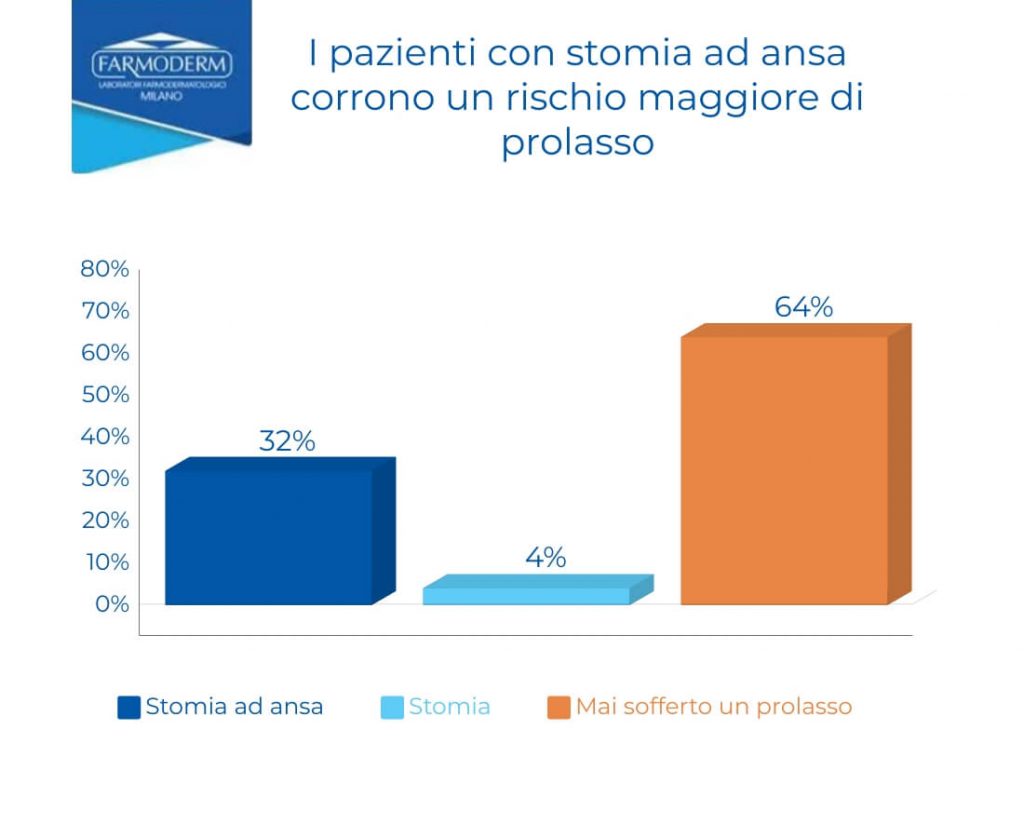
*This survey was conducted in May 2021 and was answered by 22 people of different nationalities. The survey was posted in the following ostomy-specific Facebook group: “Ileostomy,colostomy, stoma and bowel support.”
How do I cast a prolapsed ostomy?
In most cases, stomal prolapse management can be performed by the patient himself.
Often, prolapsed stoma resolves on its own. But if not, here are some things you can do if you notice the stoma protruding more than usual:
- Lie down for 20 minutes. This allows the abdominal muscles to relax and reduces pressure around the abdominal region.
- Apply gentle pressure on the prolapsed end of the stoma. This may allow the bowel to re-enter, if the stoma is not swollen.
- If the prolapse appears swollen, use a cold pack, that is, ice cubes in a plastic bag wrapped with a towel for no more than 5 minutes. Apply the pack on top of the ostomy bag.
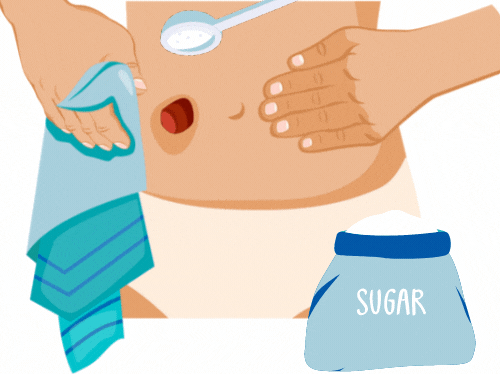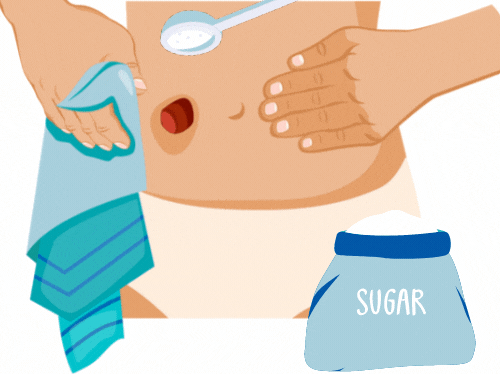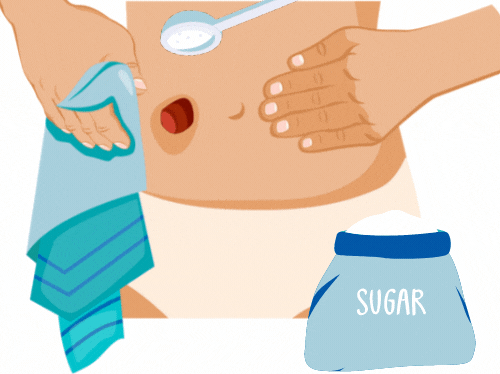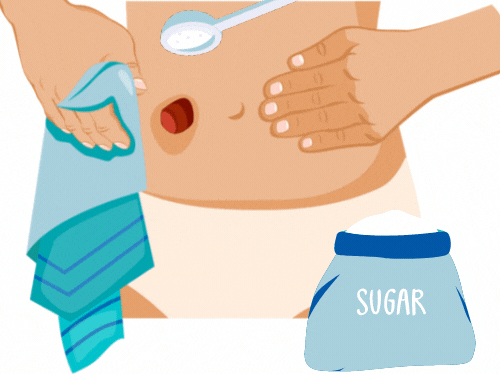
- Some ostomates use caster sugar to reduce swelling. One must apply copious amounts of caster sugar to the stoma and leave it for 20-30 minutes. Caster sugar works by absorbing fluids around the stoma. This reduces swelling and makes it easier for prolapse to return to the abdominal cavity.
- After the prolapse has been retracted, use an ostomy support belt that is specific to the prolapse.
Finally, remember to take care of the peristomal skin. In fact, ostomised people often face even severe skin changes due to improper hygiene routines, which cause itching, pain and make them feel more uncomfortable showing those parts of the body, for example at the beach or in intimacy, because they are irritated. With a proper hygiene routine, including ostomy-specific products, you will see noticeable improvements in the skin, which will remain smooth and elastic.

When to contact your doctor
Even when you decide to take care of your prolapsed ostomy on your own, it is important to keep your doctor and ostomatherapist informed so that they know what is going on and can monitor your condition. Your doctor/stomatherapist will be more familiar with your individual case and can give you specific recommendations for your treatment.
However, go to the hospital if any of the following occur:
- Prolapse appears to be purple, blue, dark red, or light pink; color changes can be a clear sign that your stoma is not getting enough oxygen and that you need to go to the hospital. Prolapse is manageable if the ostomy looks flushed and moist.
- The prolapse is cold to the touch; if the prolapse appears to be cold to the touch, it means that it is below body temperature and may also indicate that it is not getting enough blood.
- The prolapse is swollen and neither a cold compress nor granulated sugar is helpful; this indicates a more serious underlying problem and you should go to the hospital.
- The prolapse lasts for more than an hour and none of the actions taken help to resolve the problem; this may indicate a serious underlying problem and should be examined in the hospital.
- Prolapse is painful; when this happens, contact your referring physician.
If the stoma prolapse is very pronounced, surgical intervention will be needed. Surgery can be performed using local anesthesia. The process involves resection of the prolapsed part of the bowel and restructuring of the stoma to prevent recurrence of prolapse.
How can I prevent ostomy prolapse?
If you have never had a prolapse but are afraid of developing one, or if you have already had a prolapse and do not want it to happen again, you can do the following things:
- Avoid physical exercises that require excessive exertion and heavy lifting: doctors generally recommend not lifting anything over 10 pounds.
- Be careful not to gain too much weight.
- Wear an ostomy support belt that is prolapse-specific.
- Talk to your primary care physician and ask him or her which ostomy care is best for you.
- Keep your immunity up through a healthy and balanced diet, and exercise, so you can prevent troublesome symptoms such as the flu or cough.
Exercise is very important for people with an ostomy. In fact, light, regular and consistent physical activity will reduce physical recovery time while strengthening your abdominal muscles, thus preventing the risk of developing peristomal hernias and prolapses of the stoma.
In addition to physical activity, it is also important to maintain good nutrition.
Living with a prolapse: what should I do?
Although a prolapsed ostomy is not dangerous, it does require some changes in your daily routine and in the way you care for your ostomy. Here are some things you need to keep in mind to best manage a prolapsed stoma:
- You may need a larger bag to contain both prolapse and effluent.
- It may be necessary to empty or change the bag more often.
- Adjust the opening of the adhesive plate or use a moldable plate, if the prolapse is very mobile: if it slides in and out depending on your position (lying down or standing), it can increase the risk of your ostomy suffering a rubbing injury.
- You need to protect the prolapse from external trauma. Anything can cause external trauma, from leaning against a hard surface, contact sports or even hugging family and friends. Ostomy protectors, such as prolapse-specific support belts can be very helpful, depending on the size of your ostomy.
- Consider using a one-piece system .. Some two-piece systems can damage the prolapse, either by direct contact, rubbing against the prolapse, or by entrapment of some stomal surfaces between the pouch and the adhesive plate.
- Clothing may need to be adjusted to prevent clothing from rubbing against the ostomy and causing injury. Never wear belts or straps directly over the ostomy, regardless of whether you have a pouch or not.
A prolapsed ostomy can be scary; but after reading this article, you should be able to prevent and manage prolapse, with peace of mind.
Always remember that you are not alone; online you can meet many people who have had or have an ostomy and are willing to share their experience with other ostomates. Take a look at this article, if you are looking for other ostomates with whom to share your thoughts.
In addition, the use of specific stoma cleansing products, such as Bioderm Stoma Plus, is essential. This cleanser beats any conventional product in that it prevents and even reduces irritation and accelerates healing of the peristomal skin.Still haven’t found the answer to your question? We have collected the most frequently asked questions related to ostomy prolapse for you:
Frequently asked questions
Is stomal prolapse an emergency?
Although stomal prolapse is not necessarily a problem , if it lasts for more than an hour, appears blue, purple or dark red, is cold to the touch or causes you severe pain, it could be an emergency. In any of these cases, you should visit a hospital as soon as possible.
How much should a stoma protrude?
On average, the stoma protrudes about 2.5 to 3.5 cm. Many people with a colostomy experience a protrusion of about 1.5 to 2.5 cm. In general, you should talk to your referring physician about what the normal parameters are, depending on your case. Usually, a protrusion greater than usual is considered a stomal prolapse.
Is it normal for an ostomy to change size?
Your stoma will still be swollen immediately after surgery, and as it heals, it is normal for its size to change. Your ostomy will probably shrink about 6-8 weeks after surgery and even more 4-6 weeks after discharge from the hospital.
What are the causes of stomal prolapse with an ileostomy?
Although prolapses can occur after any type of surgery, the risk of developing a prolapse with an ileostomy is very low; ostomates who have a loop colostomy suffer from it especially. Nevertheless, there are various causes, such as pregnancy, obesity, heavy exercise, coughing or excessive sneezing.
